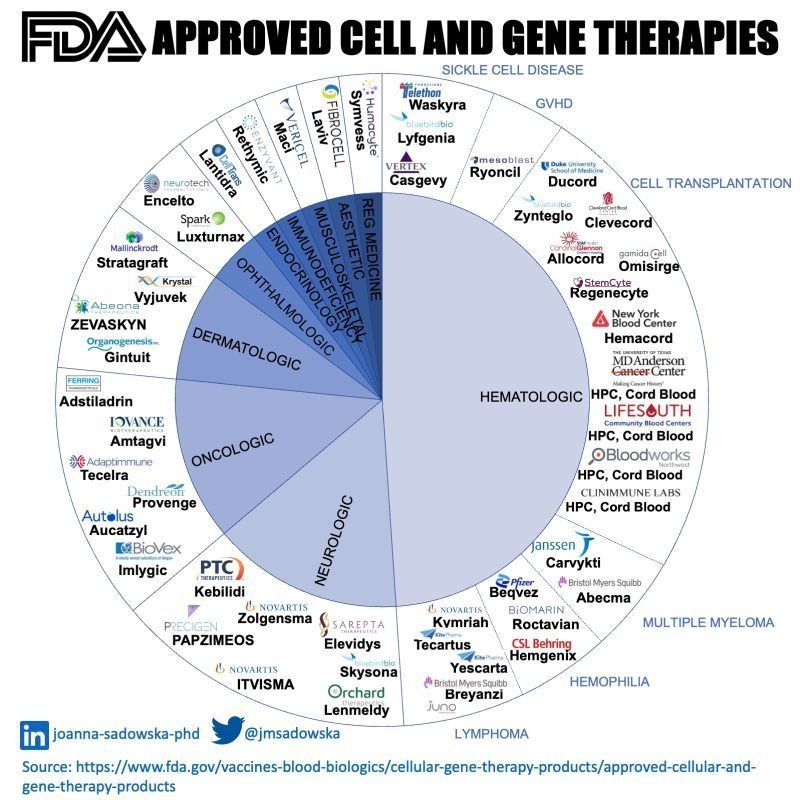
The FDA-approved cell and gene therapies are revolutionizing how we treat complex diseases, offering hope where traditional treatments fall short. These advanced therapies harness the body’s own biological machinery to correct genetic defects, regenerate damaged tissues, and fight aggressive illnesses like cancer and rare genetic disorders. With increasing approvals from the U.S. Food and Drug Administration, these cutting-edge treatments are no longer experimental—they’re becoming standard care for select patients.
Unlike conventional drugs that manage symptoms, cell and gene therapies aim to address root causes at the cellular or genetic level. From CAR T-cell therapies that reprogram immune cells to target cancer, to gene replacements that restore missing proteins, the scope is vast and growing. As research accelerates and regulatory pathways evolve, the number of FDA-approved cell and gene therapies continues to rise, marking a new era in precision medicine.
How Do FDA-Approved Cell and Gene Therapies Work?
Cell therapies involve introducing living cells into a patient to repair or replace damaged tissues. Gene therapies, on the other hand, modify or replace faulty genes to restore normal function. Both approaches are highly personalized and often used when other treatments have failed.
For example, in CAR T-cell therapy—a type of cell therapy—a patient’s T-cells are extracted, genetically engineered in a lab to recognize cancer cells, and then reinfused. This method has shown remarkable success in treating certain blood cancers like leukemia and lymphoma. Similarly, gene therapies such as Luxturna use a harmless virus to deliver a functional copy of a gene to retinal cells, restoring vision in patients with inherited blindness.
- Cell therapies: Use modified or donor-derived cells to treat disease.
- Gene therapies: Deliver corrected genes to target cells using viral vectors or other delivery systems.
- Combination approaches: Some therapies blend both strategies for enhanced effectiveness.
Breakthroughs in FDA-Approved Cell and Gene Therapies
Over the past decade, the FDA has approved a growing number of cell and gene therapies, particularly for rare and life-threatening conditions. These approvals reflect rigorous clinical testing and a commitment to patient safety. Notable examples include Zolgensma for spinal muscular atrophy and Kymriah for pediatric acute lymphoblastic leukemia.
These therapies are not without challenges. Manufacturing is complex, costs are high, and long-term effects are still being studied. Yet, their potential to deliver cures—not just symptom relief—sets them apart. The FDA’s accelerated approval pathways, such as Breakthrough Therapy and Regenerative Medicine Advanced Therapy (RMAT) designations, help bring these innovations to patients faster.
Recent advances also include gene editing tools like CRISPR, which allow for precise modifications to DNA. While still largely in clinical trials, CRISPR-based therapies could soon join the ranks of FDA-approved cell and gene therapies, expanding treatment options for conditions like sickle cell disease and beta thalassemia.
Who Benefits from These Therapies?
The primary beneficiaries of FDA-approved cell and gene therapies are patients with rare genetic disorders, certain cancers, and degenerative diseases. These therapies are often one-time treatments with the potential for long-lasting or even curative effects.
For instance, patients with Leber congenital amaurosis (LCA), a rare inherited eye disease, have regained functional vision thanks to gene therapy. Similarly, individuals with severe combined immunodeficiency (SCID), often called “bubble boy disease,” can now live normal lives after gene correction.
However, access remains a challenge. High costs—sometimes exceeding $1 million per treatment—limit availability. Insurance coverage varies, and logistical hurdles in cell collection and processing add complexity. Still, patient advocacy and policy efforts are working to improve equity and affordability.
Key Takeaways: The Future of FDA-Approved Cell and Gene Therapies
- The FDA-approved cell and gene therapies represent a paradigm shift in medicine, moving from chronic management to potential cures.
- These therapies are highly specialized, often targeting rare diseases and cancers with unmet medical needs.
- Regulatory support from the FDA, including expedited review pathways, is accelerating innovation.
- Challenges remain in manufacturing scalability, cost, and long-term monitoring, but progress is steady.
- Ongoing research in gene editing and delivery systems promises even more breakthroughs in the coming years.
Frequently Asked Questions
What is the difference between cell therapy and gene therapy?
Cell therapy involves transplanting or modifying living cells to treat disease, while gene therapy focuses on correcting or replacing defective genes within cells. Both can be used together in advanced treatments.
Are FDA-approved cell and gene therapies safe?
Yes, all FDA-approved cell and gene therapies undergo rigorous clinical trials to ensure safety and efficacy. However, like any medical treatment, they carry risks, including immune reactions and long-term uncertainties, which are closely monitored.
Can these therapies cure diseases permanently?
In many cases, yes. Some FDA-approved cell and gene therapies offer durable or potentially curative outcomes, especially for genetic disorders and certain cancers. Long-term follow-up studies continue to assess lasting benefits.
The landscape of medicine is evolving rapidly, and the FDA-approved cell and gene therapies are at the forefront of this transformation. As science advances and regulatory frameworks adapt, these therapies will likely become more accessible, affordable, and effective—ushering in a new age of healing that was once thought impossible.