The inflammatory response is one of the most fundamental protective mechanisms in human biology. It allows the body to detect injury, fight infection, and begin the process of tissue repair. Without inflammation, even minor wounds or routine bacterial exposure could become life threatening.
At the same time, when the inflammatory response becomes excessive or chronic, it can contribute to a wide range of diseases including arthritis, cardiovascular disease, diabetes, autoimmune disorders, and neurodegeneration. Understanding how this process works, what triggers it, and how it is regulated is essential for both medical professionals and health conscious individuals.
This article provides a detailed, practical overview of the inflammatory response, including its stages, key cellular players, benefits, risks, and clinical relevance.
What Is the Inflammatory Response
The inflammatory response is the body’s immediate biological reaction to harmful stimuli such as:
-
Pathogenic microorganisms
-
Physical injury
-
Chemical irritants
-
Tissue necrosis
-
Immune system activation
It is part of the innate immune system and occurs rapidly, often within minutes of injury or infection.
The primary goals of the inflammatory response are to:
-
Eliminate the initial cause of cell injury
-
Remove damaged tissue and pathogens
-
Initiate tissue repair
-
Restore normal function
Types of Inflammatory Response
Inflammation is commonly classified into two major forms based on duration and function.
Acute Inflammatory Response
This is the short term, rapid reaction that occurs within hours or days.
Characteristics include:
-
Redness
-
Heat
-
Swelling
-
Pain
-
Temporary loss of function
Common examples include inflammation around a cut, sprained ankle, or bacterial infection.
Chronic Inflammatory Response
This develops when inflammation persists for weeks, months, or years.
It is associated with:
-
Continuous immune cell infiltration
-
Ongoing tissue destruction
-
Fibrosis or scarring
-
Altered organ function
Chronic inflammation is implicated in conditions such as rheumatoid arthritis, inflammatory bowel disease, asthma, and atherosclerosis.
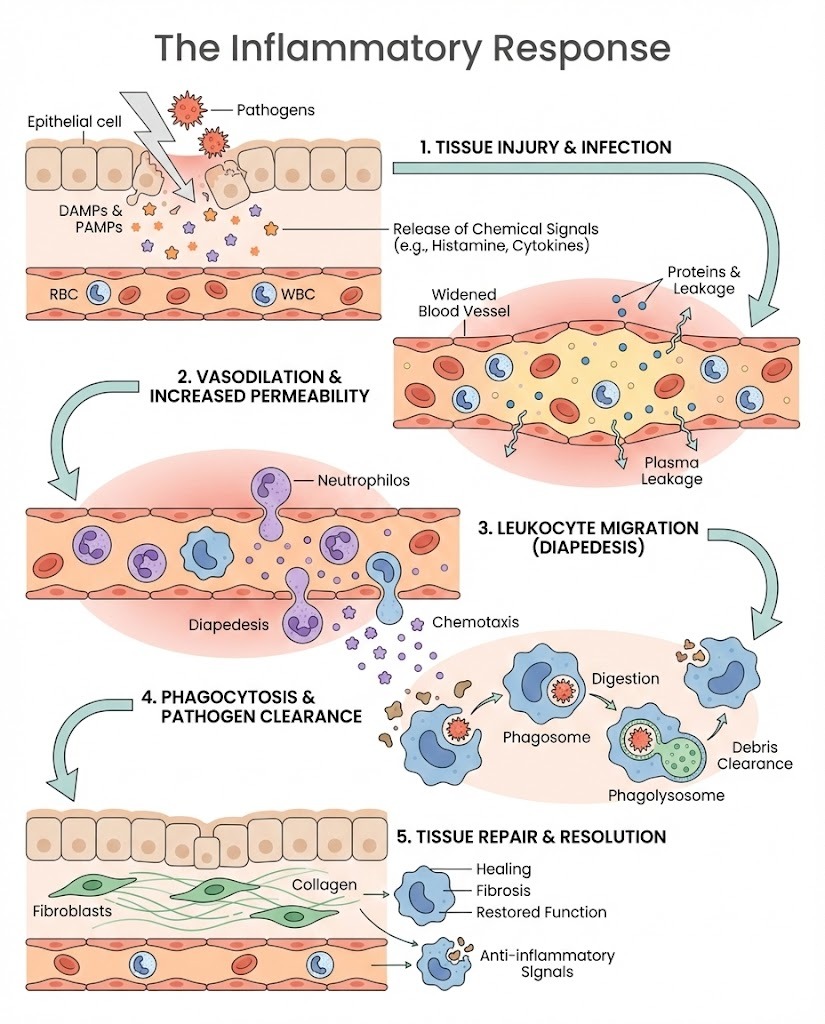
Stages of the Inflammatory Response
The inflammatory response follows a predictable sequence of biological events.
1. Recognition of Injury or Pathogen
Specialized immune cells detect:
-
Microbial components
-
Damaged cell molecules
-
Foreign particles
These signals activate inflammatory pathways.
2. Release of Chemical Mediators
Cells release substances such as:
-
Histamine
-
Prostaglandins
-
Cytokines
-
Chemokines
-
Bradykinin
These mediators increase blood vessel permeability and attract immune cells to the affected area.
3. Vascular Changes
Blood vessels undergo:
-
Vasodilation leading to redness and warmth
-
Increased permeability causing swelling
These changes allow immune cells and proteins to reach damaged tissue.
4. Cellular Response
White blood cells migrate to the site, primarily:
-
Neutrophils in early stages
-
Macrophages in later stages
Their role is to:
-
Engulf pathogens
-
Remove debris
-
Release additional signaling molecules
5. Resolution and Repair
Once the threat is eliminated:
-
Inflammatory signals decrease
-
Dead cells are cleared
-
Tissue regeneration begins
-
Normal structure is gradually restored
Failure of this stage can lead to chronic inflammation.
Key Cells Involved in the Inflammatory Response
Several immune cells coordinate the inflammatory process.
-
Neutrophils rapidly attack bacteria and fungi
-
Macrophages remove debris and orchestrate later immune activity
-
Mast cells release histamine and initiate vascular changes
-
Dendritic cells present antigens to adaptive immune cells
-
Lymphocytes contribute during prolonged or immune specific inflammation
Each cell type plays a distinct role in shaping the magnitude and duration of the response.
Molecular Pathways That Drive Inflammation
The inflammatory response is controlled by complex signaling networks.
Important pathways include:
-
Nuclear factor kappa B signaling
-
Cyclooxygenase enzyme pathways
-
Complement system activation
-
Toll like receptor signaling
Modern anti inflammatory drugs often target these molecular mechanisms to reduce symptoms and tissue damage.
Benefits of the Inflammatory Response
When properly regulated, inflammation is essential for survival.
Key benefits include:
-
Rapid elimination of infectious agents
-
Prevention of pathogen spread
-
Efficient wound healing
-
Activation of adaptive immunity
-
Removal of damaged cells
Without inflammation, even minor injuries could progress into severe systemic infections.
Risks of Excessive or Chronic Inflammation
Problems arise when the inflammatory response becomes uncontrolled.
Potential consequences include:
-
Tissue destruction
-
Organ dysfunction
-
Autoimmune reactions
-
Increased cancer risk
-
Accelerated aging processes
Chronic inflammation has been linked to:
-
Heart disease
-
Alzheimer’s disease
-
Type 2 diabetes
-
Obesity related metabolic disorders
-
Certain cancers
This dual nature makes inflammation both protective and potentially harmful.
Measuring the Inflammatory Response in Clinical Practice
Healthcare professionals evaluate inflammation using:
-
C reactive protein levels
-
Erythrocyte sedimentation rate
-
White blood cell count
-
Cytokine profiling
-
Imaging studies for tissue swelling
These markers help diagnose infection, monitor chronic disease, and assess treatment effectiveness.
Managing and Modulating Inflammation
Medical strategies aim to reduce harmful inflammation while preserving its protective role.
Common approaches include:
-
Nonsteroidal anti inflammatory drugs
-
Corticosteroids
-
Immunosuppressive therapies
-
Biologic agents targeting specific cytokines
Lifestyle factors also influence inflammatory status:
-
Balanced nutrition
-
Regular physical activity
-
Adequate sleep
-
Stress management
-
Avoidance of smoking
Research continues to explore dietary components such as omega 3 fatty acids, polyphenols, and fiber for their potential anti inflammatory effects.
The Inflammatory Response in Modern Medicine
Advances in immunology have transformed how inflammation is understood and treated.
Current areas of investigation include:
-
Personalized anti inflammatory therapies
-
Biomarker guided treatment plans
-
Immune system modulation rather than suppression
-
Targeted biologic medications
-
Links between inflammation and neurodegenerative disease
These developments highlight the central role of the inflammatory response in both acute care and chronic disease management.
Conclusion
The inflammatory response is a vital biological process that protects the body from injury and infection while initiating tissue repair. Through a coordinated sequence of cellular and molecular events, it eliminates harmful stimuli and restores physiological balance.
However, when this response becomes excessive or prolonged, it can contribute to serious chronic diseases and long term tissue damage. Understanding how inflammation functions, how it is regulated, and how it can be safely controlled remains a cornerstone of modern medicine.
A balanced inflammatory response is not merely a sign of illness but a critical indicator of how effectively the body defends and heals itself.
Frequently Asked Questions
What is the inflammatory response in simple terms
The inflammatory response is the body’s natural reaction to injury or infection. It brings immune cells and protective chemicals to damaged tissue to fight harmful agents and begin healing.
What triggers the inflammatory response
It can be triggered by bacteria, viruses, physical injury, toxins, autoimmune reactions, or damaged cells releasing distress signals.
How is chronic inflammation different from acute inflammation
Acute inflammation is short term and resolves after healing. Chronic inflammation persists for long periods and can cause tissue damage and contribute to disease development.
Can the inflammatory response be harmful
Yes. While it is essential for protection, excessive or long lasting inflammation can damage healthy tissues and increase the risk of conditions such as heart disease, arthritis, and neurodegenerative disorders.